Articular Cartilage: An Overview of Structure and Function
Dr. Shruti Bajad
Common advice treats joints like simple hinges. Biology is less forgiving. When I examine a synovial joint, I see articular cartilage performing quiet, complex work that keeps motion smooth and pain low. It is basically a living, load-bearing surface. In this overview, I outline how its structure underpins its performance, and why small changes cascade into symptoms.
Structure of Articular Cartilage
Four Distinct Zones of Articular Cartilage
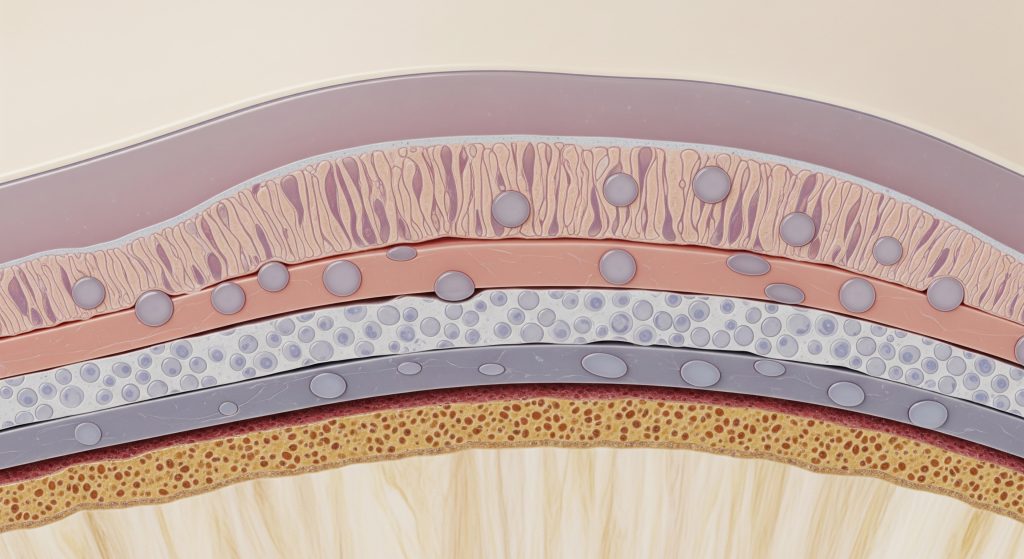
Healthy articular cartilage is stratified into four zones arranged from surface to bone. Each zone has a distinct fibre pattern and cell behaviour that suits its mechanical role. The layering matters because load, fluid flow, and shear vary with depth.
|
Zone |
Key features |
|---|---|
|
Superficial (tangential) |
Parallel collagen fibres, flattened chondrocytes, high water content, low permeability. |
|
Middle (transitional) |
Oblique fibres, rounded cells, higher proteoglycans, energy dissipation. |
|
Deep (radial) |
Perpendicular fibres, columnar cells, highest proteoglycans, strong compressive support. |
|
Tidemark and calcified |
Mineralised layer anchoring cartilage to subchondral bone, mechanical coupling. |
Cellular Components and Chondrocytes
Chondrocytes are the resident cells that maintain the matrix. I think of them as careful stewards rather than prolific builders. They regulate collagen and proteoglycan turnover, respond to mechanical cues, and adjust synthesis with age or injury. Density is low, so disrupted signalling has outsized effects. Small error, large consequence.
Extracellular Matrix Composition
The extracellular matrix provides most mechanical strength. Water occupies a large fraction and moves under load. Type II collagen forms the tensile scaffold. Aggrecan and other proteoglycans bind water to generate osmotic swelling pressure. The balance between collagen tension and swelling governs stiffness and resilience.
Collagen Network Organisation
Collagen fibres are arranged in a depth-dependent arc. Parallel at the surface to resist shear. Oblique in the middle to diffuse stress. Perpendicular near bone to anchor and channel load. This architecture distributes forces efficiently and preserves surface integrity under repetitive motion.
Functions of Articular Cartilage
Load Distribution and Shock Absorption
Articular cartilage spreads compressive loads across the joint contact area. Under load, fluid is expressed slowly, and proteoglycan swelling counteracts compression. In practice, this biphasic behaviour attenuates peaks and protects deeper tissues. I often describe it as a fluid pressurised mattress with a fibre net on top.
Friction Reduction During Joint Movement
The surface presents an exceptionally low friction interface. Boundary lubricants and a smooth collagen network limit shear. Interstitial fluid pressurisation further reduces contact of solid surfaces. This is where articular cartilage function is most visible to patients as effortless movement.
Protection of Underlying Bone
By absorbing and redistributing energy, articular cartilage shields subchondral bone from high strain. The calcified zone and tidemark form a secure junction that resists delamination under cyclical loads. When cartilage thins, bone adapts. Sometimes painfully.
Nutrient Exchange Mechanisms
Articular cartilage is avascular, so transport relies on diffusion and fluid convection during loading. Joint motion enhances exchange of glucose, oxygen, and waste through the matrix and synovial fluid. Moderate, regular loading is beneficial here, provided inflammation is controlled.
Conclusion
Structure dictates performance. The zonal design, sparse chondrocytes, and finely tuned matrix enable articular cartilage to bear load, reduce friction, and protect bone with minimal wear. Damage disrupts this synergy. Early intervention, careful loading, and targeted rehabilitation help preserve function while longer term options are considered. The aim is simple. Keep the surface intact for as long as possible.
Frequently Asked Questions
What is the thickness of healthy articular cartilage?
Thickness varies by joint and region, typically a few millimetres in load-bearing areas. The patellar and femoral condylar surfaces often present greater thickness than smaller joints.
Can articular cartilage regenerate naturally?
Intrinsic repair is limited because the tissue is avascular and cell density is low. Small superficial defects may stabilise, but full structural restoration is uncommon without intervention.
What nutrients are essential for articular cartilage health?
Glucose and oxygen support chondrocyte metabolism, delivered via synovial fluid. Adequate vitamin D and protein intake aids overall joint health, though local mechanics remain decisive.
How does ageing affect articular cartilage function?
Ageing reduces proteoglycan content and alters collagen crosslinking, which changes stiffness and resilience. Cellular responsiveness declines to an extent, slowing matrix turnover and repair.
What is the difference between articular cartilage and other types of cartilage?
Articular cartilage is hyaline cartilage designed for low friction loading at synovial joints. Fibrocartilage, by contrast, tolerates tensile stress, while elastic cartilage supports flexible structures.







 We do what's right for you...
We do what's right for you...



